2.11.0
Does the Dorsal Shutdown Create Dissociation, as the Polyvagal Theory proposes?
What is Dissociation?
The Merriam and Webster dictionary offers two definitions: a chemical process and a psychological process. It describes a chemical process in which bound molecules break apart. Psychologically, we can think of dissociation in terms of perception (fragmented or distorted perception) or identity (splitting the personality into different parts).
Etymology
Dissociation (dis+sociation = separate) is the opposite of association (ad+sociation = unite), and both terms are built around the root soc- as in social, sociology, or socialism. The Latin “socius” was a companion or ally in war.
What does the PVT say?
The PVT postulates that the dorsal vagus (DVC) produces dissociation and associates it with metabolic shutdown and immobility in an unavoidable situation. Reducing dissociation to a collapsing process of numbness and immobility is wrong. Here, we show other perspectives.

Dissociation in the chemical sense: The splitting of water into hydrogen and oxygen.
2.11.1
Psychotraumatology and Dissociation
Few psychological concepts have been as controversial as dissociation. Introduced by the French psychologist Pierre Janet, dissociation remained unquoted for decades until the rise of psychotraumatology in the late 1980s brought it back to life. Since then, the two leading psychotraumatology societies (ISSTD and ESTD) have made it clear that dissociation is related to psychotrauma. Among several authors, van der Hart, Nijenhuis, and Steele (The Haunted Self) insisted that complex PTSD belongs to dissociative disorders and not to anxiety disorders, as previously thought. The three authors proposed a return to Pierre Janet's original writings to regain conceptual clarity. They coined the term “structural dissociation of the personality” to emphasize that dissociation involves a division of the whole personality into subsystems or parts (Nijenhuis, 2019).
Dissociation is an acute or chronic state in which a person ceases to experience themselves as a complete, embodied person. Their conscious experience is divided or interrupted, and they may lose voluntary control over certain cognitive or physical processes. People who dissociate may feel consciously disconnected from their sense of self, body, thoughts, feelings, memories, and behaviors. Breuer and Freud, a century ago, described “hysterical” manifestations (e.g., paralysis) that were later called “dissociative.”
Porges doesn't define dissociation properly and reduces it to a part of the “dorsal” shutdown. This ignores a century of research (from Janet to structural dissociation). It doesn't take into account the role of cortical areas. It confuses “freezing” and dissociation. Therefore, PVT is not an appropriate tool or working framework for treating dissociative disorders.
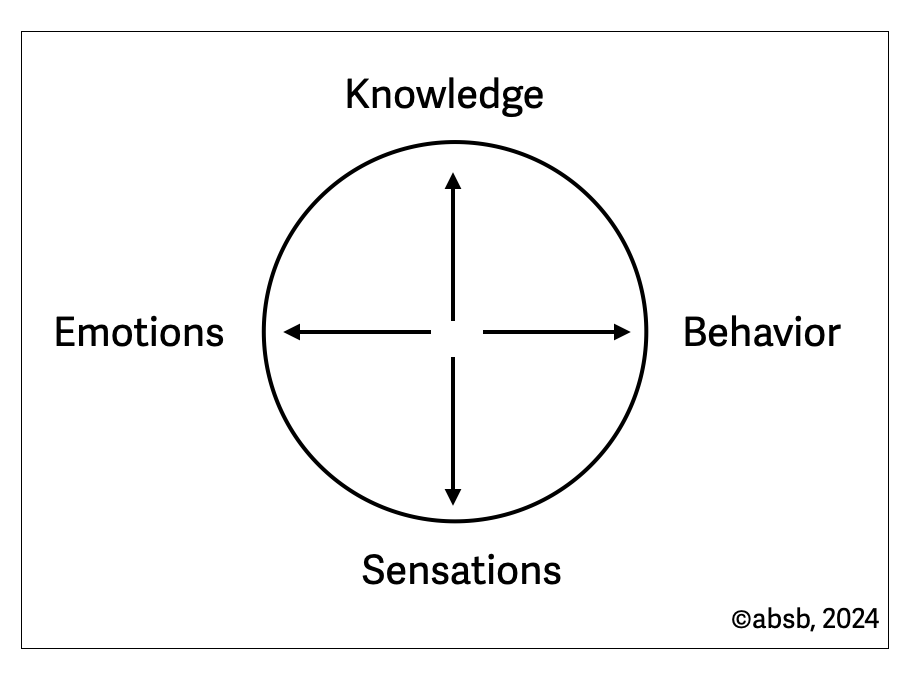
Graphic interpretation of the BASK Model as a wheel
The BASK Model of Dissociation (Braun, 1988) is based on four axes: sensations, emotions, knowledge, and behavior. Braun describes how the various functions can fail in traumatic circumstances. Interestingly, it includes the somatoform disorders described by Nijenhuis (2004), which are disturbed sensations (e.g., numbness) or impaired mobility (e.g., paralysis).
Following Different Types of “Dissociation” Have Different Psychological Mechanisms (Brown, 2006), most experts in psychotraumatology agree on the distinction between two types of post-traumatic dissociation:
detachment, as in derealization and depersonalization
compartmentalization, as in Dissociative Identity Disorder (DID).
Are there two qualitatively distincts forms of dissociation? (Holmes, 2005). Yes, there are.
The Bask model explains that dissociation is not a functional decrease or shutdown. It's a lack of integration. Let's take an example. The famous Belgian writer Amélie Nothomb describes in Biographie de la faim (2004) (Life of Hunger, 2006) how she lost the ability to calculate after being raped as a teenager-this is dissociation. Dissociation means that a person can't put their sh* together-feeling, thinking, and acting in one place, as usual. The brilliant lady Nothomb can still write bestsellers, but she can't calculate anymore because of those stupid rapists in the Indian Ocean. There is no place for “dorsal gibberish” here — it is cortical!
2.11.2
Neurobiology of the Dissociation
Modular dissociation
The brain has 86 billion neurons organized into modular networks. As the word “network” implies, they operate interconnected. Although a single module generates specific information, each must eventually be integrated with other modules, creating extended networks throughout the brain (e.g., salience, default, or focused modes). A “small world pattern” distinguishes between local and long-range connections. See Networks of the Brain (Sporns, 2011).
When neural modules connect, they can also disconnect, resulting in a dissociated experience. Thus, the brain has two ways to produce dissociation: deactivating a module (which is easily detected by functional studies such as fMRI or PET) or disconnecting modules in a connectome (an ensemble of connections).
“Watching a movie with only a brain module for vision—without access to the one for emotions—would detract greatly from the experience” (Bertolero, 2019) in How the Mind Emerges from the Brain’s Complex Networks.
In Deep posteromedial cortical rhythm in dissociation (Vesuna, 2020), the authors investigate the dissociative effect of ketamine. A research team with Vesuna observed the effect of ketamine and found a 1-3 Hz rhythm in the retrosplenial cortex. They found that rhythmic optogenetic activation of the retrosplenial cortex produced a dissociation-like behavioral effect. In a patient with focal epilepsy, simultaneous intracranial encephalography revealed a similar rhythm in the deep posteromedial cortex that correlated with self-reported dissociation. Brief local electrical stimulation of this region elicited dissociative experiences. According to The dissociative and analgesic properties of ketamine are independent (Gitlin, 2020), ketamine's channel-blocking activity at NMDA receptors may explain its dissociative properties.
2.11.3
Hypnosis: A Helpful Dissociation
Technical dissociation
A third group has its roots in hypnosis — e.g., Hilgard (1975, 1977) and Milton Erickson. Bandler and Grinder — developers of NLP (Neurolinguistic Programming), introduced the concept of “technical dissociation” (or even double dissociation according to Bandler), which is often used in brief therapy techniques (EFT and psychotrauma therapy).
In the second half of the last century, various therapists, especially hypnotherapists and NLP therapists, have explored dissociation as a technique of desensitization. A “technical dissociation” takes advantage of dissociation's protective or adaptive effect. A Third-Person Perspective (3-PP) technique can rapidly resolve a simple trauma. Steve and Connirae Andreas, both students (1977) of Bandler, had created a one-day clinic based on this principle.
Hypnosis
Unlike the technical dissociation discussed above, classical hypnosis generally produces states of trance characterized by deep muscular relaxation, decreased sensitivity to pain, and increased suggestibility. Subjects remain conscious and awake. It has been shown that a change in cerebral connectivity, rather than opioid mechanisms, is the explanation for the decreased pain. Similar phenomena have been observed in The neural mechanisms of mindfulness-based pain relief (Zeidan, 2015, 2016, 2019).
Hypnosis decouples cognitive control from conflict monitoring processes of the frontal lobe (Egner, 2005)
Functional neuroanatomy of the hypnotic state (Faymonville, 2006)
Neurophysiology of hypnosis (Vanhaudenhuyse, 2014)
2.11.4
Neuroimaging & Structural Dissociation

We find here the same distinction between dissociation as a perceptual disorder and dissociation as an identity disorder. Some neuroscientists, such as Reinders, focus on DID (dissociative identity disorder), showing different profiles of brain activation consistent with specific behaviors (e.g., adaptive, aggressive, or submissive behaviors). Others, such as Vesuna (2020), have studied dissociation as a disturbed perception.
While the phenomenon is still not fully understood and remains a subject of debate and research, there have been studies using neuroimaging techniques (fMRI) to examine changes in brain activity associated with different personality states in DID patients.
More articles by Simone, Reinders, Nijenhuis, Schlumpf, Jäncke, at al.
Dissociative Part-Dependent Resting-State Activity in Dissociative Identity Disorder (Schlumpf, 2014) reports that different identity states in individuals with DID are associated with distinct patterns of neural activity during the retrieval of traumatic memories.
Psychobiological Characteristics of Dissociative Identity Disorder: a symptom provocation study ((Reinders, 2006), the authors describe how different patterns of brain activation appear (different identities) when patients listen to trauma-related scripted imagery. Conclusions: Patients with DID encompass at least two distinct DIS. These identities are associated with different subjective reactions, cardiovascular responses, and cerebral activation patterns to a trauma-related memory script.
Opposite brain emotion regulation patterns in identity states of dissociative identity disorder: A PET study and neurobiological model (Reinders, 2014). Imaging studies of PTSD reveal distinct neural network patterns between hypoaroused/dissociative and hyperaroused subtypes. The authors propose a neurobiological model of DID based on two PTSD subtypes:
Overmodulation of emotion regulation: rostral/dorsal anterior cingulate, prefrontal cortex, posterior association areas, and parahippocampal gyri.
Undermodulation of emotion regulation: amygdala and insula, dorsal striatum
This supports the notion that DID is related to PTSD, as hypoaroused and hyperaroused states are similar in DID and PTSD.
A PET study and neurobiological model (Reinders, 2014). This study shows how dissociative identity disorder (DID) involves different emotional states or different brain activation patterns (hyper - vs. hypo-aroused) in PTSD. Monitoring the brain with PET (positron emission tomography) shows that:
the hypo-aroused identity state activates the prefrontal cortex, cingulate, posterior association areas, and the parahippocampal gyri (overmodulating emotion regulation)
the hyper-aroused identity state activates the amygdala, insula, and dorsal striatum (undermodulating emotion regulation).
Dissociative Part-Dependent Resting-State Activity in Dissociative Identity Disorder: A Controlled fMRI Perfusion Study (Schlumpf, 2014)
Aiding the diagnosis of dissociative identity disorder: pattern recognition study of brain biomarkers (Reinders, 2019). The authors identified patterns that could accurately discriminate between individuals with DID and healthy controls. These findings provide evidence for a biological basis for distinguishing DID from healthy individuals. This is important and clinically relevant because the diagnosis of DID is controversial and individuals with DID are often misdiagnosed. Ultimately, the application of pattern recognition methods could prevent unnecessary suffering of individuals with DID through earlier accurate diagnosis, allowing for faster and more targeted interventions.
Dissociative identity disorder: out of the shadows at last? (Reinders, 2021)
2.11.5
Do Opioids Cause Dissociation?
Short answer: Although endogenous opioids (endorphins) can create a dissociative state (e.g., numbness, derealization, or depersonalization), their role is relatively limited. As clinical research shows, the effect of opioid antagonists on chronic dissociation is not fully convincing. Other cortical mechanisms (disconnection between brain regions) seem more likely to create these specific states. The hypnotic management of the pain, which appears to be a sort of dissociation, is not influenced by opioid antagonists.
In Neurobiology and Treatment of Traumatic Dissociation toward an Intended Self (Lanius, Paulsen, Corrigan, 2014), Lanius strongly suggests that opioids cause dissociation. In Chapter 5, Dissociation and Endogenous Opioids: A Foundational Role, Lanius begins with this statement: There is little doubt that dissociation is at least in part mediated by endorphins and endogenous opioids (e.g., Scaer, 2001; Schore, 2001).» Consequently, various researchers have explored the possibility of reducing the effects of opioids.
Treatment with low-dose naltrexone
Opioid overdose causes respiratory arrest, leading to death. Therefore, the use of an opioid antagonist (e.g., naltrexone, Narcan, naloxone) should effectively treat dissociative symptoms. However, the results of studies — especially in Germany — are not entirely conclusive.
Naltrexone in the treatment of dissociative symptoms in patients with borderline personality disorder: an open-label trial (Bohus, 1999)
These observations support the hypothesis that increased activity of the opioid system contributes to dissociative symptoms, including flashbacks, in borderline personality disorder and that these symptoms may respond to treatment with opiate antagonists.
LDN- Niedrig dosiertes Naltrexon (on German)(Pies, 2010).
Low dose naltrexone in the treatment of dissociative symptoms (Pape, 2015)
A Medication to Gain Self-Awareness: Treatment of Dissociative Symptoms in Trauma-Related Disorder II Video + article (Pape 2017). Treatment with low-dose naltrexone may be a helpful element in the treatment of patients with complex post-traumatic stress disorder. However, it is important to recognize that the reduction in dissociation may present patients with an unresolved challenge, as dissociation may have previously been a necessary self-protective mechanism.
The relationship between dissociative symptoms and medications used to treat opioid use disorder (Gainer, 2021). This study shows that individuals taking prescribed buprenorphine have higher mean dissociation symptom scores than those taking prescribed methadone and naltrexone. Higher DES scores are also significantly associated with more recent opioid use, less time on medication, depression symptoms, and PTSD scores.
Altered Central — Opioid Receptor Binding After Psychological Trauma (Liberzon, 2007)
Current Understanding of the Neural Mechanisms of Dissociation in Borderline Personality Disorder (Krause-Utz, 2018)
Dissociation in Borderline Personality Disorder: Recent Experimental, Neurobiological Studies, and Implications for Future Research and Treatment (Krause-Utz, 2021)
2.11.6
Polyvagal Theory and Dissociation
Consistent with the PVT, a fourth group of authors adhere to an animal model description, conflating dissociation with immobilization, metabolic shutdown, and faking death.
While the term “dissociation” was absent from the Polyvagal Theory Index (2011), it appears fourteen times in the Polyvagal Safety Index (2021). Dissociation is then associated with immobility or numbness (p. 200) or is next to “syncope, fainting, and defecation” (p. 257).
Many authors and Internet bloggers paint a similar picture (e.g., Rege, 2023). This is problematic for several reasons.
1. PVT is based on a mammalian immobilization model, anatomically located in the brainstem. In this setting, dissociation is synonymous with immobility, metabolic shutdown (hibernation-like), and bradycardia.
2. Immobility refers to the somatic motor system. It describes an adaptive behavior activated from the midbrain PAG (or higher) via myelinated nerves terminating at the striated skeletal muscles. Being immobile doesn't imply dissociation. Conversely, patients describe going about their usual business while in a dissociative state of emotional numbness. This may be an “apparently normal part of personality” (ANP) (van der Hart, 2006) or a case of depersonalization and derealization.
An artist can give a concert, or a soldier can run under enemy fire in a dissociated state. While paralysis, which used to be called hysteria or conversion disorder, is on the list of possible dissociative symptoms, it's not mandatory. Similarly, numbness refers to the afferent somatic system–a sensory deprivation. It is not vagal. Recently, Porges has begun to talk a lot about how victims cannot fight back during the attack (peritraumatic paralysis) and feel ashamed afterward. This can undoubtedly happen, but unfortunately, the list of dissociative symptoms is much longer, and “immobility” isn't automatically one of them.
3. Metabolic shutdown, similar to motor inhibition, is not mandatory in dissociation. This would mean a drop in temperature, thyroid hormone, catecholamine, and blood sugar. The role of the dorsal complex (DVC) is to protect and stabilize the metabolism (homeostasis), not to shut it down.
4. As seen in the chapter “Ventral,” the heartbeat control depends on the ventral parasympathetic branch (NAext). It down-regulates the frequency (chronotropic) negative of the sinoatrial node discharge and the propagation speed to the atrioventricular node (dromotropic negative). Recent research shows that the ventral vagal branch causes bradycardia. The DVMN (dorsal vagal motor nucleus), in addition to metabolic, immune, and visceral functions, protects the ventricles from sympathetic overdrive (inhibition of adrenergic tone). It uses N02 as a transmitter, causes coronary dilatation, and suppresses inflammatory processes due to heart damage (stroke).
5. PVT postulates an autonomic causality in the discussion on dissociation. It confuses visceral functions with motor and cognitive functions. An animal model cannot describe the full complexity of human dissociation. Taking the debate to the cortex is critical.
6. The PVT describes dissociation as an energetic pushdown rather than a division, as most clinicians (cf. Janet) see. It doesn’t consider the lack of integration.
N.B. Various authors, such as Porges (2021, p. 249), place dissociation and depression in a line, blaming “the dorsal.” However, we have known for decades that depression is a serotonin and noradrenaline (norepinephrine) problem. Again, there is confusion among the systems.
2.11.7
How does Polyvagal Theory Impact Research?
Here, we briefly present some studies on dissociation published by authors influenced by the PVT. The third (Kearney, Lanius 2022) avoids referencing the PVT but instead cites MacLean, which is usually a bad omen. We are not surprised when the authors postulate an ontogenetic-phylogenetic connection at the cranial nerve VIII (vestibular) level, recalling a similar development by Porges about the vagal nerve.
fMRI functional connectivity of the periaqueductal gray in PTSD and its dissociative subtype (Harricharan, Schore, Ruth Lanius, et al. 2016). In this PVT-influenced article, the authors examine the connectivity of the PAG (periaqueductal gray) in dissociative disorders. The dissociative subtype of PTSD, characterized by depersonalization and derealization symptoms, is often accompanied by additional passive or submissive defensive responses associated with autonomic blunting. The authors attempt to support Porges' arguments by incorrectly assuming that the PAG plays a role in threat detection. The PAG is more involved in executing behavioral responses to threats under the direction of the amygdala and higher brain centers than in directly assessing threats (amygdala or ACC).
A Review of the Neurobiological Basis of Trauma-Related Dissociation and Its Relation to Cannabinoid- and Opioid-Mediated Stress Response: a Transdiagnostic, Translational Approach (Ruth Lanius et al., 2018, p.4). According to polyvagal theory, immobilization, and death feigning are thought to occur due to activation of the DVC and its inhibitory inputs to the heart, associated with immobilization, bradycardia, and apnea (Porges, 2011).
The brain-body disconnect: A somatic sensory basis for trauma-related disorders (Kearney, Ruth Lanius, 2022). At first glance, this article is free of polyvagal references, which is surprising for an article co-authored by Ruth Lanius. However, a closer look reveals that the authors describe how «the brain retained its older structures and reorganized them with each cortically directed evolutionary step, similar to the ontogenetic pattern of neurodevelopment .» Later, they quote MacLean’s (1985) triune brain theory, «suggesting the brain to be a phylogenetically layered system that began with the “reptilian” or subcortical brain. Upon the foundation of subcortical structures developed the limbic system, now nestled within the cortical midline and heavily involved in emotion and self-related processing.» In different parts of the article, the authors describe the importance of the vestibular system in dissociation therapy. They postulate an early phylogenetic and ontogenetic development of the VIII cranial nerve — earlier than other cranial nerves. For us, there's a slight whiff of “recapitulation.”
Trauma-related dissociation and the autonomic nervous system: a systematic literature review of psychophysiological correlates of dissociative experiencing in PTSD patients (Beutler, 2022). Beutler extensively quotes Porges and the PVT: « Through this framework, dissociative responding in humans is purely a defensive immobilization response modulated by the dorsal vagal complex and associated with large heart rate decreases. This immobilization response occurs when behaviors initiated by the ventral vagal complex (e.g. social engagement) or the sympathetic-adrenal pathway (e.g. active defensive behavior) are not possible.»
2.11.8
Further Reading on Dissociation
Peritraumatic dissociation revisited: associations with autonomic activation, facial movements, staring, and intrusion formation (Danböck, 2021).
Seventy-one healthy women watched a highly aversive movie. At the same time, autonomic activation (heart rate, respiratory sinus arrhythmia, skin conductance level), facial movements (temporal variations in “corrugator electromyography”), and gaze (fixation duration, track length) were assessed. Participants then rated the intensity of dissociation during movie viewing and reported intrusions. Peritraumatic dissociation was associated with higher autonomic arousal (higher heart rate and lower RSA, increased facial movements and staring (lower track length)) and higher intrusion distress.
Heterogeneity of defensive responses after trauma exposure: blunted autonomic reactivity in response to startling sounds (D'Andrea, 2013)
Dissociation (e.g., shutting down or "spacing out") correlates with unresponsiveness and blunted arousal. These clinical features suggest that the possibility of threat responses other than fight/flight, namely immobilization, may be underpinned by hyper- or hypoarousal. Autonomic responses to a stressful stimulus (acoustic startle) are observed: heart rate acceleration, deceleration, and skin conductance response. The students showed heterogeneous responses:
Blunted reactivity, with decreased acceleration and skin conductance, and increased deceleration in individuals with significant symptoms and early exposure to multiple types of trauma.
Significant heart rate acceleration and skin conductance responses in individuals with subclinical symptoms and more attenuated exposure.
Dissociation following traumatic stress: Etiology and treatment (Schauer, 2010). «We suggest that trauma treatment must, therefore, differentiate between patients on two dimensions: those with peritraumatic sympathetic activation versus those who went down the whole defense cascade, which leads to parasympathetic dominance during the trauma and a corresponding replay of physiological and dissociative responding when reminded.»
Our comment: this corroborates the observations made by Peter Levine (1997), comparing the active versus passive behavior of survivors in Chowchilla. His work provokes a physical mobilization with concomitant activation of the sympathetic system to emerge from the pattern of immobility.
Sleep Deprivation Induces Acute Dissociation via Altered EEG Rhythms Expression and Connectivity (Menicucci, 2022). Acute sleep deprivation promotes dissociative experiences by creating a state of consciousness that is facilitated by higher large-scale synchronization at high frequencies.
Dissociation and Brain Rhythms: Pitfalls and Promises (Grent-'T-Jong, 2021)
>> to the next chapter Dorsal Vagal Shutdown